You may have been told your NK cells are high. Your clinic has recommended intralipids — an intravenous fat infusion offered before transfer to calm the immune response that may, the theory goes, be working against your embryo.
The test felt like an answer after so many cycles without one. A measurable marker. An explanation. And now a treatment to address it.
The Human Fertilisation and Embryology Authority, the UK’s independent fertility regulator, formally assesses the add-ons offered alongside standard IVF. Their evidence reviews are used internationally by clinicians and patients trying to understand what the research actually shows.
Intralipids are on that list.
What intralipids are
Intralipids are an intravenous emulsion of soybean oil, egg phospholipids, glycerin and water — originally developed as nutritional support for patients unable to eat. In fertility, they are used off-label as an immune modulator.
The proposed mechanism is that the lipid components of the infusion interact with immune cells — particularly natural killer cells — and suppress their activity around the time of transfer, creating a more tolerant uterine environment for the embryo.
The infusion is administered intravenously, typically in the days before transfer and sometimes repeated in early pregnancy. Unlike IVIG, intralipids are relatively inexpensive and carry a lower risk profile — which is partly why they are offered more readily and earlier in the treatment pathway.
What NK cells actually do
Natural killer cells have a name that implies they are a problem to be solved. In the context of implantation, that framing is misleading.
Uterine NK cells are essential to successful implantation. They are the most abundant immune cells in the uterus during the implantation window and the early stages of pregnancy. They support vascular remodelling — the process by which new blood vessels form to supply the developing placenta. They guide trophoblast invasion — the process by which the embryo embeds into the uterine lining. They contribute to placental formation and help regulate the immune tolerance that allows the embryo to remain without being rejected.
The question is not whether NK cells are present. They should be. The question is whether their activity is dysregulated in a way that interferes with implantation — and that is a different question entirely from whether a blood test shows an elevated count.
The problem with peripheral NK cell testing
The NK cell test most commonly offered before intralipids measures natural killer cells in peripheral blood — a sample taken from the arm.
Peripheral blood NK cells and uterine NK cells are distinct populations with different phenotypes, different functions and different regulatory mechanisms. An elevated count in the blood does not reliably predict elevated or dysregulated activity in the uterus. The two populations do not behave the same way, are not regulated by the same signals, and cannot be read as equivalent.
A high result on a peripheral NK cell test tells you that NK cell levels in your blood are elevated. It does not tell you what your uterine NK cells are doing — or whether intralipids would have any meaningful effect on the environment your embryo is being transferred into.
This distinction is not a minor technical point. It is the reason the evidence for intralipid treatment based on peripheral NK cell testing remains limited.
What the regulator assessment shows
The HFEA reviews each add-on against the evidence for whether it improves the chance of a live birth.
On intralipids, the published assessment is that the evidence is insufficient — there is not enough high-quality trial data to support or reject routine use. Unlike IVIG, which carries a red rating due to safety and efficacy concerns, intralipids sit in grey: the signal is unclear, the safety profile is relatively benign, and the research is ongoing.
The grey rating does not mean intralipids are ineffective. It means the evidence has not yet reached the threshold required to make a reliable recommendation either way.
The clinical situations where intralipids may be considered are specific:
- Recurrent implantation failure where immune dysregulation has been identified by a reproductive immunologist through uterine assessment — not peripheral blood testing alone
- Women with a diagnosed autoimmune condition where immune modulation has a documented clinical rationale
- Women with endometriosis, where chronic pelvic inflammation may contribute to a dysregulated uterine immune environment
If intralipids were offered on the basis of a peripheral NK cell blood test alone, without a reproductive immunologist’s assessment of uterine immune activity, the regulator’s assessment is useful information to bring into the conversation with your clinic.
The regulator’s work is designed to inform that conversation, not replace it.
What intralipids cannot reach
Intralipids modulate the immune environment from outside — delivered intravenously, acting systemically. What shapes the uterine immune environment from within is a different set of inputs entirely.
The inflammatory tone of the uterus responds to gut health, metabolic patterns, blood sugar stability, dietary fat quality and micronutrient status. Vitamin D modulates uterine NK cell activity and supports the immune tolerance that implantation depends on. Omega-3 fatty acids reduce systemic inflammatory signalling. Selenium and zinc support immune regulation at the cellular level. These are the nutritional inputs that influence whether the uterine environment is pro-inflammatory or tolerant — and none of them are addressed by an intravenous infusion.
Intralipids act on the immune system from outside. The nutritional environment shapes it from within.
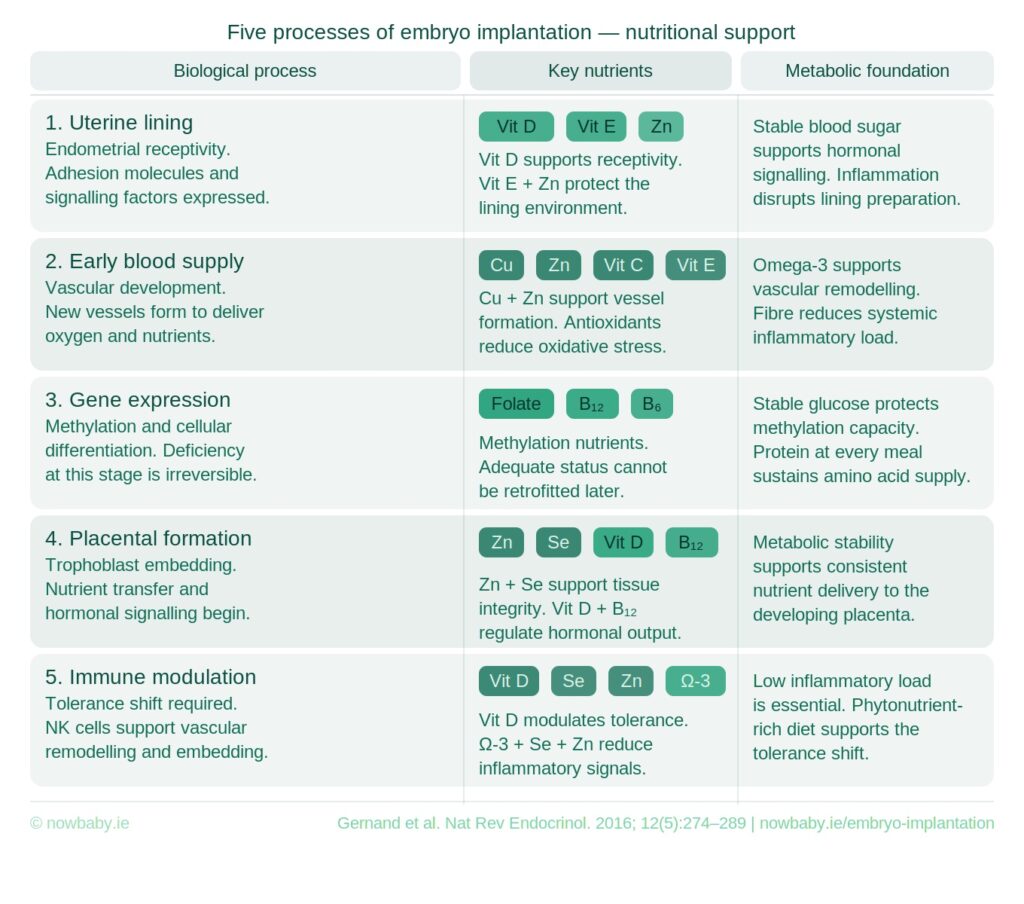
More than 1 in 3 frozen transfers do not result in a live birth. Embryo implantation has 5 distinct phases and each has its own nutrient requirements. Your embryo needs to complete uterine lining preparation, early blood supply, gene expression, placental formation and immune modulation — all before a test can confirm anything. Each of those phases responds to what the body has been given to work with.
The Now Baby FET Implantation Meal Plan was designed around every one of those phases — the nutritional structure for the days your biology is doing its most demanding work. Professionally analysed. Beginning the day after transfer.

You didn’t come this far to wing it.