The baby you are working toward begins with biology that is both precise and quietly extraordinary. Ovulation can feel like a monthly event — one egg, released, then gone. But egg development is not a one-month story. If you have been told your numbers look acceptable, yet pregnancy has not happened, it is often because the visible monthly event is only the final stage of a much longer process.
The egg involved in a future pregnancy has been developing, signaling, and responding to its environment for months — and, in some respects, for years — before ovulation ever occurs.
Here we will trace egg development from the primordial follicle to ovulation.
Egg Development Begins Before Birth
All the eggs a woman will ever have are formed during fetal life. By around mid-pregnancy, the ovaries contain a peak number of immature eggs, and from that point onward, no new eggs are made. Instead, the existing pool gradually declines.
Before birth, most of these eggs are lost. At birth, a smaller pool remains. By puberty, that pool has fallen further. Each immature egg is enclosed in a primordial follicle — the most basic structural unit of the ovary.
At this stage, the egg has entered the first phase of meiotic division and then paused.
This pause — known as meiotic arrest — is a normal and essential part of human reproduction. The egg does not continue dividing. Instead, it remains held in a stable, suspended state, sometimes for decades, until the signal to resume development occurs just before ovulation.
What Is Meiosis and Why It Matters for Egg Quality
Meiosis is the specialised form of cell division that produces eggs and sperm.
Its role is to halve the genetic material in reproductive cells so that, when egg and sperm combine, the resulting embryo has the correct number of chromosomes.
In egg development, meiosis begins before birth and then pauses part-way through the first division. That pause can last for decades. Maintaining chromosome integrity and cellular organisation over such a long time is one reason egg quality is sensitive to the conditions within the ovary. When fertilisation occurs but pregnancy does not continue, this prolonged meiotic pause is part of the biology worth understanding.
From Dormant to Active: Follicle Recruitment
At any given time, a small number of primordial follicles are recruited to begin development. This recruitment is continuous and is initially regulated largely by local ovarian signalling rather than by reproductive hormones from the brain.
At any one time, only a small subset of the total follicle pool is recruited into active growth, and it is this limited group of developing follicles that contributes to the antral follicle count and produces measurable levels of anti-Müllerian hormone (AMH).
Primary Follicle Stage
In the primary follicle, the egg begins to grow and become metabolically active.
Key changes include:
- Enlargement of the egg
- Activation of ribonucleic acid (RNA) and protein synthesis
- Changes in surrounding support cells (granulosa cells)
The egg remains in meiotic arrest, but it is no longer dormant. It becomes increasingly dependent on its micro-environment for energy, protection, and signalling.
Secondary Follicle Stage
As the follicle develops into a secondary follicle:
- Granulosa cells multiply and organise
- The zona pellucida (a protective glycoprotein layer around the egg) forms
- Communication channels between the egg and granulosa cells increase
At this stage, the egg does not function independently. It relies on surrounding cells to supply nutrients, manage oxidative stress, and coordinate growth and timing. This cooperative relationship is essential: changes in the health of support cells affect the egg directly.
Antral Follicle Stage and Hormonal Sensitivity
The next major transition is the formation of the antral follicle. A fluid-filled cavity (the antrum) develops, and the follicle becomes responsive to reproductive hormones, particularly follicle-stimulating hormone (FSH).
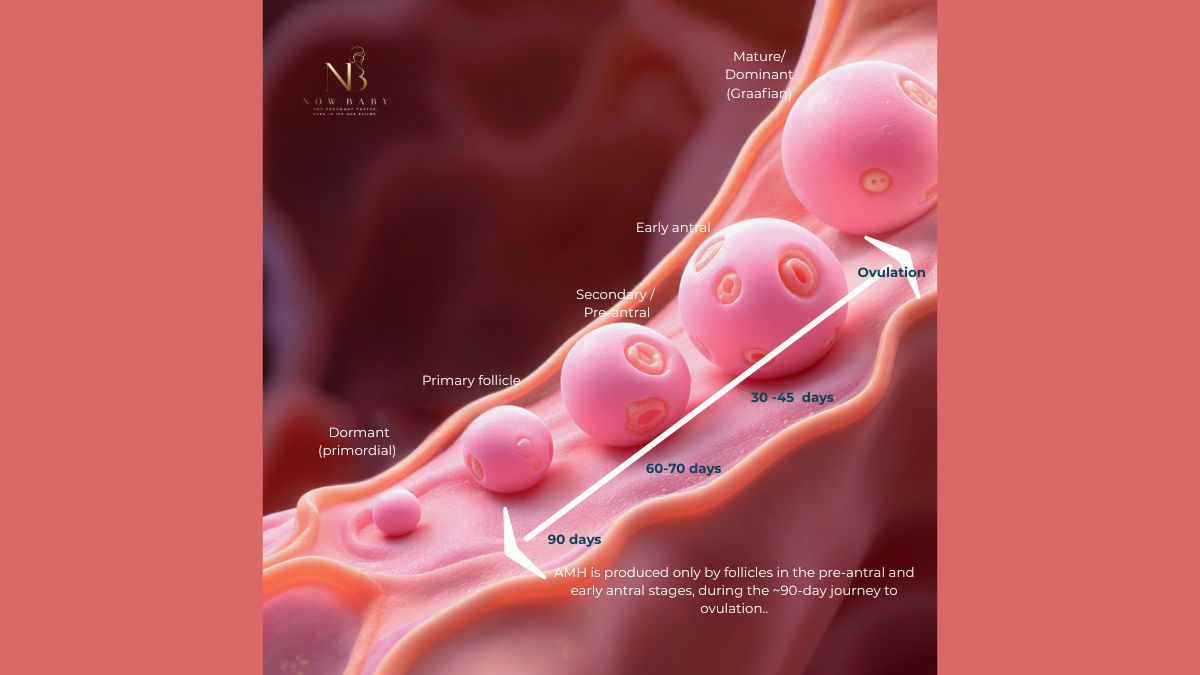
Anti-Müllerian hormone (AMH) is produced by granulosa cells of small growing follicles, particularly in the pre-antral and early antral stages, where it reflects local follicular activity rather than egg quantity. A low AMH result reflects signalling within currently developing follicles — it does not measure the total number of eggs remaining.
This is the stage assessed during antral follicle count scans. It is also the stage that becomes visible and measurable in many fertility work-ups.
One key point holds: these follicles did not begin developing “this month.” They have been progressing toward this stage over a longer biological timeline.
Selection of the Dominant Follicle
During a natural cycle, one antral follicle becomes dominant. This follicle continues growing while others regress.
Dominance is not random. It reflects how efficiently a follicle responds to hormonal signals and how robust its internal support system is — cellular, metabolic, and structural — built over time.
Ovulation and Completion of Meiosis I
Just before ovulation, a surge in luteinising hormone (LH) triggers the egg to resume meiosis.
At this point:
- Meiosis I is completed
- A small package of genetic material called the first polar body is expelled
- The egg enters meiosis II, where it pauses again
Ovulation releases an egg that is metabolically active and time-sensitive. Meiosis II will only complete if fertilisation occurs.
After ovulation, the follicle does not simply disappear. The granulosa cells (along with theca cells) undergo a transformation called luteinisation, forming the corpus luteum — a temporary gland that produces progesterone to support the luteal phase and help prepare the uterine lining for implantation.
Why Egg Quality Is About Time, Not Just Age
Egg quality is often discussed as a function of age alone. Age matters — but it is not the whole story.
Egg quality reflects:
- How long the egg has been held in meiotic arrest
- The integrity of cellular structures over time
- The health and signalling capacity of supporting follicular cells
- The metabolic and inflammatory environment during development
This is why egg quality is not something that can be meaningfully “fixed” in a single cycle. Ovulation is the visible moment of a longer process.
What Shapes the Ovarian Environment
The ovarian environment is not abstract. It reflects systemic physiology — metabolic stability, inflammatory load, micronutrient sufficiency, and mitochondrial capacity within supporting cells.
These influences operate quietly over time. They are rarely visible in a single blood test or scan, yet they shape the conditions in which follicles develop.
What This Means for Fertility Care
When we understand egg development, the frame shifts. We frequently see women who have been reassured that ovulation is occurring normally, yet the deeper developmental window has never been reviewed. Fertility stops being only about monthly pressure or isolated numbers and becomes about respecting biological timelines and supporting the conditions that shape cellular health over time.
In our fertility consultations, we examine this longer developmental timeline — not just ovulation on a scan, but the biological conditions that have shaped the egg over preceding months, particularly when cycles look “normal” but pregnancy has not followed
Egg development is not something that happens to you in one month. It is something your body has been doing consistently, carefully, for years.
Nature’s Wisdom
If you are waiting — for a cycle, a scan, a result, or a next step — know this: your body is not idle. Work is already underway in the same way it has been for every woman before you.
Ovulation is only the visible moment of a much longer, hidden process.